Covid Testing & Autoimmune Disease
Autoimmune Disease Can Cause False-Positive Antibody Test Results
A just-published study shows systematic false-positive antibody test results for patients with certain auto-immune diseases across a wide range of commercial SARS-CoV-2 serological assays. Specifically for patients with rheumatoid arthritis or lupus, but NOT multiple sclerosis.
These are the blood-based antibody tests used to determine if a person has previously been exposed to the SarsCoV2 virus. This is NOT the PCR-based tests used to diagnose someone with a current viral infection.
Patients in the Study Group
The pool of test subjects were people diagnosed with one of three autoimmune diseases:
Rheumatoid Arthritis
Systemic Lupus Erythematosus
Multiple Sclerosis
Antibody Tests Used in the Study
The study looked at 17 commercially available lateral flow assays (LFA), two ELISA kits, and one in-house developed multiplex bead-based assay. The lateral flow assays are the disposable pin-prick drop-of-blood tests that look like pregnancy tests. The ELISA and bead-assay tests are laboratory-run antibody tests requiring a full blood-draw.
These tests are designed to be highly specific to JUST antibodies generated from a SarsCoV2 infection. They target two different categories of antibodies, the IgG and IgA antibodies. Here are the commercial test examined in the study:
Research Results
Patients with rheumatoid arthritis or lupus consistently showed false-positives for SarsCoV2 IgM antibodies, but NOT for SarsCoV2 IgA antibodies.
Multiple Sclerosis patients showed no false-positives on either IgM or IgA antibody assays.
These results do NOT appear to imply any sort of protective mechanism for rheumatoid arthritis or lupus patients but rather an artifact of how the underlying antibody tests have been designed.
To quote the paper:
It could be argued that the unspecific signals detected in this study might actually be due to some underlying immunity, if there are mechanisms such as molecular mimicry behind the triggering of autoimmunity and these would also, hypothetically, work in the reverse direction. However, a more plausible explanation is that it is due to a technical difficulty in the assay development and thus one should not assume that these signals confirm any immunity against infection.
Here are the core study results:
Link to the paper:
SARS-CoV-2 serological tests can generate false positive results for samples from patients with chronic inflammatory diseases
About the author:
I am a scientist with 20+ years in the biotech industry. I currently work as a consultant with companies involved in developing molecular diagnostics platforms, including some of the key testing platforms used to detect the SarsCoV2 virus.
So I bring an insider’s perspective that is scientifically oriented but directed to a general audience trying to make sense of the conflicting stories surrounding the Covid pandemic.
To learn more: https://www.linkedin.com/in/dalewharrison/
If you found this article useful, please sign up by hitting the “Subscribe Now” button below or share it with a friend…





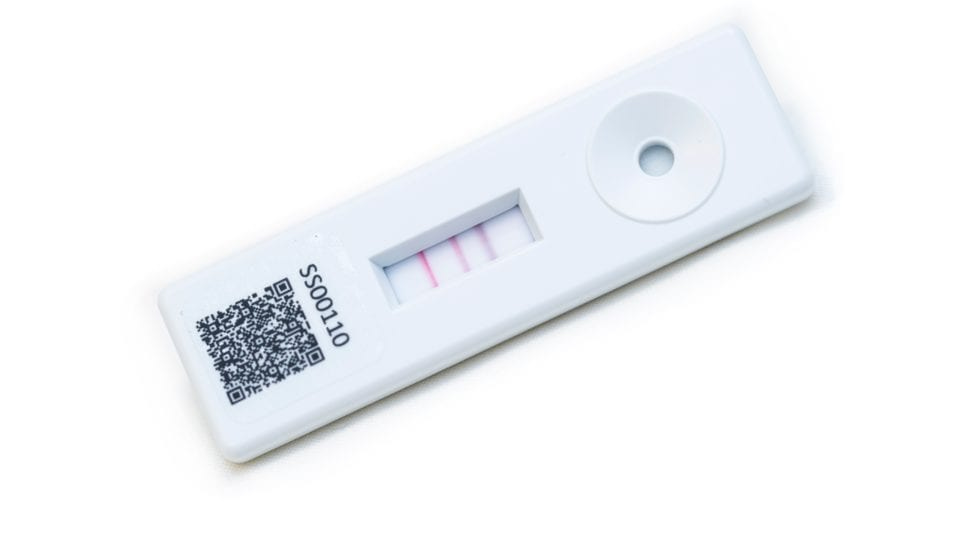



I am testing positve on every lateral flow test that I do but my PCR test is always negative. Please explain.