The US is currently seeing 430 Covid cases-per-100,000 population per week. This is a truly astonishing level of infectious spread!
In terms of your personal risk of being exposed to an infected person, it’s useful to compare this with the risk of being exposed to seasonal influenza. During a normal flu season, the equivalent risk level would 35 cases-per-100k population per week. The worse flu season in the past 25 years was only at an equivalent of about 100 cases-per-100k population per week.
So your current risk of exposure is 10x greater than in a normal flu season; more than 3x greater than the worst flu season most people have ever experienced. The current level of outbreak represents an infectious risk level beyond anything experienced in modern times…for at least a century or more!
Yesterday, December 2nd, we saw the highest recorded death toll in the US at almost 3,200 people. Over 200,000 new cases were reported with:
30 states have test-positivity rates above 10%
32 states reporting rising case levels
Whitehouse Coronavirus Task Force Report
The Whitehouse Coronavirus Task Force periodically releases a lengthy report with state-level review and guidance. The current Issue 24 dated Nov-29-2020 is 413 pages in length (link at the bottom of this article).
Their current recommendations are stark. Below are a few of the ones included in the report:
They begin with a direct rebuke to the extremely poor performance of many state governors and local officials:
If state and local policies do not reflect the seriousness of the current situation, all public health officials must alert the state population directly.
For anyone over 65 - do not enter indoor public spaces:
If you are over 65 or have significant health conditions, you should not enter any indoor public spaces where anyone is unmasked due to the immediate risk to your health; you should have groceries and medications delivered.
If you attended a Thanksgiving gathering then assume you’re already infected:
If you are under 40, you need to assume you became infected during the Thanksgiving period if you gathered beyond your immediate household.
Most likely, you will not have symptoms; however, you are dangerous to others and you must isolate away from anyone at increased risk for severe disease and get tested immediately.
A call for increased testing and identification of asymptomatic carriers:
The silent community spread that precedes and continues to drive these surges can only be identified and interrupted through proactive, focused testing for both the identification of asymptomatic and pre-symptomatic individuals. This must be combined with significant behavior change of all Americans.
A call for universal use of masks and distancing at all times:
Ensure masks at all times in public; increase physical distancing through a significant reduction in capacity in public and private indoor spaces, including restaurants and bars; and ensure every American understands the clear risks of ANY family or friend interactions outside of their immediate household indoors without masks.
Special vigilance for anyone over 65 who might have been exposed:
If you are over 65 or have significant medical conditions and you gathered outside of your immediate household, you are at significant risk for serious COVID infection
If you develop any symptoms, you must be tested immediately as the majority of therapeutics work best early in infection.
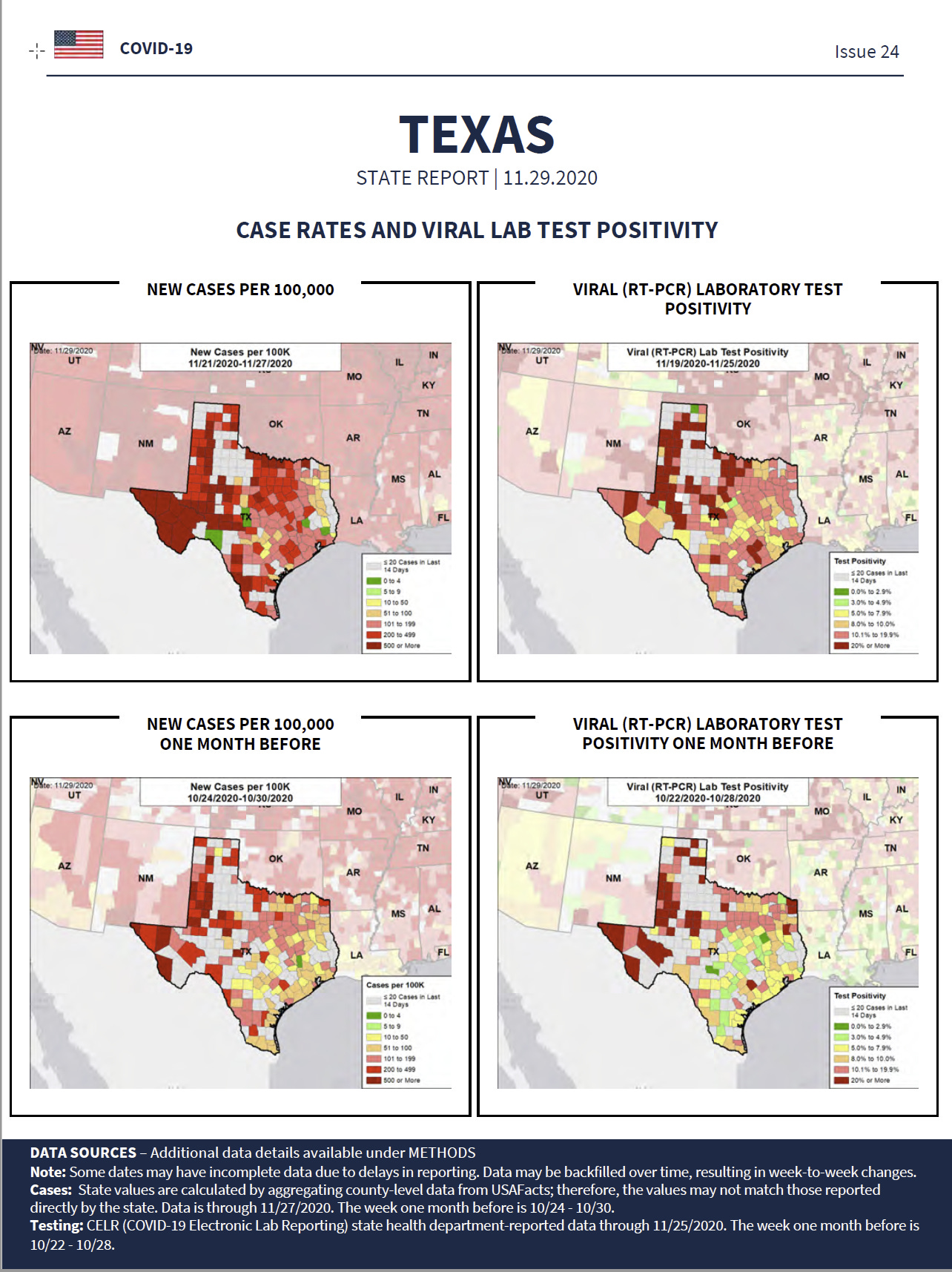
Report Summary for Texas
Texas had 248 new cases per 100,000 population – 38th highest rate in the US.
Texas has a test positivity rate at or above 10.1% – 27th highest rate in the US.
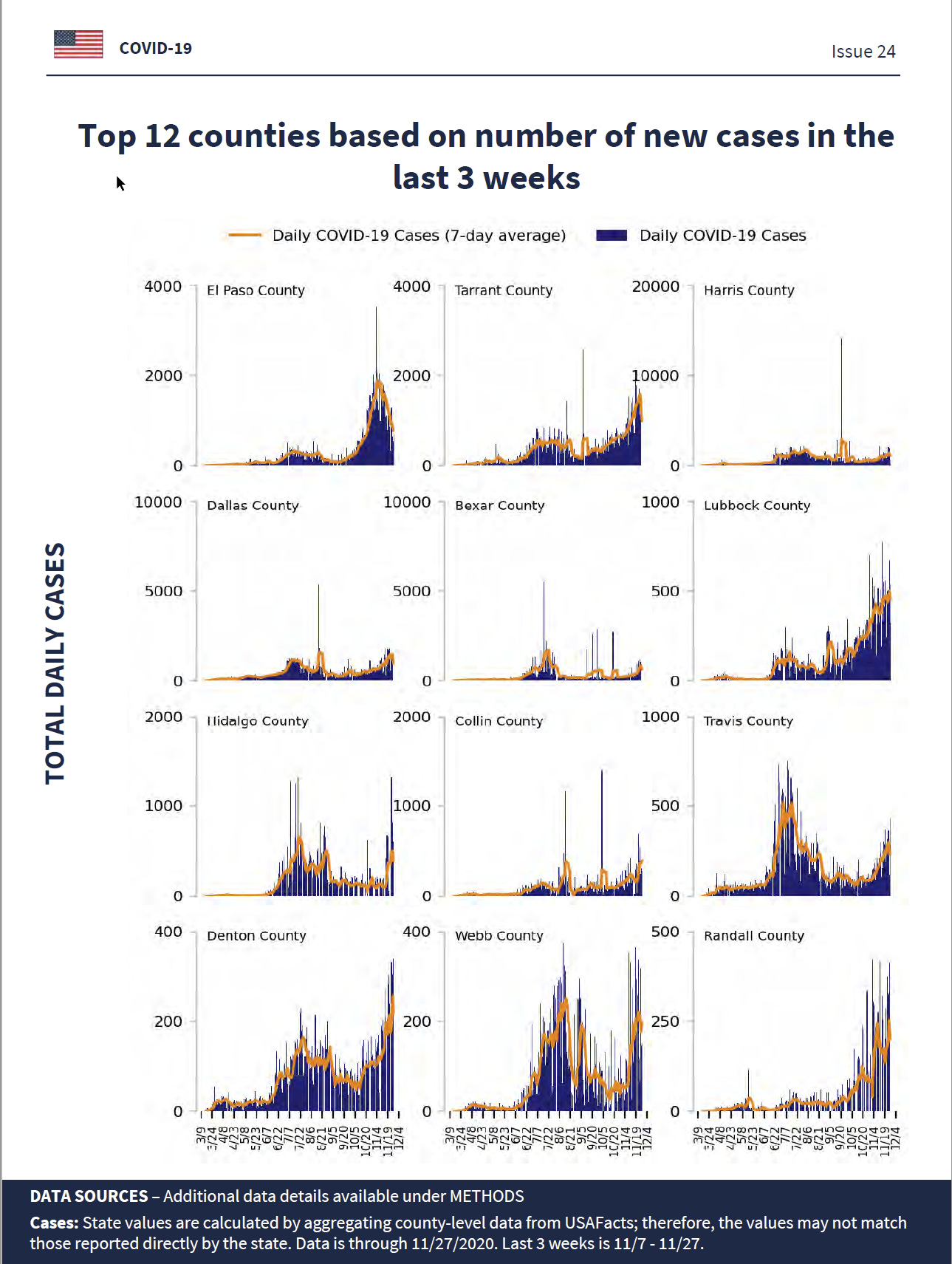
The following 3 counties have the highest number of new cases:
Paso County
Tarrant County
Harris County
These counties represent 33.5% of new cases in Texas.
During the week of Nov 16 - Nov 22 Texas had:
21% of nursing homes had at least one new resident COVID-19 case
38% had at least one new staff COVID-19 case
7% had at least one new resident COVID-19 death.
Between Nov 21 - Nov 27, on average reported as newly admitted each day to hospitals in Texas:
964 patients with confirmed COVID-19
629 patients with suspected COVID-19
Key Recommendations
The COVID risk to all Americans is at a historic high. The national daily COVID incidence after Memorial Day, but before the summer surge, was fewer than 25,000 new cases/day and is now more than 180,000 new cases/day; COVID inpatients then were fewer than 30,000 but are now more than 90,000; fatalities have more than doubled.
We are in a very dangerous place due to the current, extremely high COVID baseline and limited hospital capacity; a further post-Thanksgiving surge will compromise COVID patient care, as well as medical care overall.If state and local policies do not reflect the seriousness of the current situation, all public health officials must alert the state population directly.
It must be made clear that if you are over 65 or have significant health conditions, you should not enter any indoor public spaces where anyone is unmasked due to the immediate risk to your health; you should have groceries and medications delivered. If you are under 40, you need to assume you became infected during the Thanksgiving period if you gathered beyond your immediate household.Most likely, you will not have symptoms; however, you are dangerous to others and you must isolate away from anyone at increased risk for severe disease and get tested immediately.
If you are over 65 or have significant medical conditions and you gathered outside of your immediate household, you are at significant risk for serious COVID infection; if you develop any symptoms, you must be tested immediately as the majority of therapeutics work best early in infection.We are also seeing clear improvement in many European countries that implemented strong public and private mitigation but preserved schooling. We are also seeing states and cities that aggressively mitigated achieving a high plateau and early stability in less than 4 weeks.
However, in many areas of the USA, state mitigation efforts remain inadequate, resulting in sustained transmission or a very prolonged time to peak – over 7 weeks. All states and all counties must flatten the curve now in order to sustain the health system for both COVID and non-COVID emergencies.The silent community spread that precedes and continues to drive these surges can only be identified and interrupted through proactive, focused testing for both the identification of asymptomatic and pre-symptomatic individuals. This must be combined with significant behavior change of all Americans.
Ensure masks at all times in public; increase physical distancing through a significant reduction in capacity in public and private indoor spaces, including restaurants and bars; and ensure every American understands the clear risks of ANY family or friend interactions outside of their immediate household indoors without masks.Proactive weekly testing of groups representative of the community (teachers, community college students, county workers, staff in crowded or congregate settings, all hospital personnel, large private sector employers) will help identify the depth and breadth of community infection.
These cases should be triangulated with cases among long-term care facility (LTCF) staff to identify geographic areas with high numbers of asymptomatic and pre-symptomatic cases, which should then trigger widespread testing, identification, and isolation of positive cases among community members, stopping the ongoing spread.
These efforts to identify and reduce asymptomatic transmission should run concurrently with testing of symptomatic persons and contact tracing of cases.Expand strategic use of point-of-care antigen tests for all individuals that gather across households. Antigen tests perform well in the highly infectious window and will be effective in the identification of asymptomatic and pre-symptomatic infectious cases. Antigen tests do not perform well after 8-10 days post-infection when nucleic acid cycle times are >30.
New hospital admissions in Texas are beginning to peak. Conduct aggressive impact testing of adults under 40 to rapidly identify those who became infected over Thanksgiving before they spread the virus to more vulnerable individuals, driving another round of increased hospitalizations and fatalities.
Full Report for Texas
Link to the Full Report for All 50 States
About the author:
I am a scientist with 20+ years in the biotech industry. I currently work as a consultant with companies involved in developing molecular diagnostics platforms, including some of the key testing platforms used to detect the SarsCoV2 virus.
So I bring an insider’s perspective that is scientifically oriented but directed to a general audience trying to make sense of the conflicting stories surrounding the Covid pandemic.
To learn more: https://www.linkedin.com/in/dalewharrison/
If you found this article useful, please sign up by hitting the “Subscribe Now” button below or share it with a friend…